Over the past few decades, the world has witnessed a surge in emerging infectious diseases, many of which have emerged from wildlife and domestic animal populations to humans, causing significant global health crises. Experts estimate that over 70% of new infectious diseases emerge from animals, driven by deforestation and wildlife trade. From the devastating impact of HIV/AIDS and Ebola to the recent COVID-19 pandemic, the interconnectedness of human, animal, and environmental health has never been more apparent.
Understanding the phenomenon of zoonotic spillover, where pathogens cross the species barrier from animals to humans, is crucial for preventing future outbreaks and safeguarding global health security. In this article, we wll discuss the role of wildlife reservoirs and zoonotic disease spillover, exploring the underlying drivers, examining case studies, and outlining essential prevention and mitigation strategies.
Understanding Zoonotic Disease Spillover
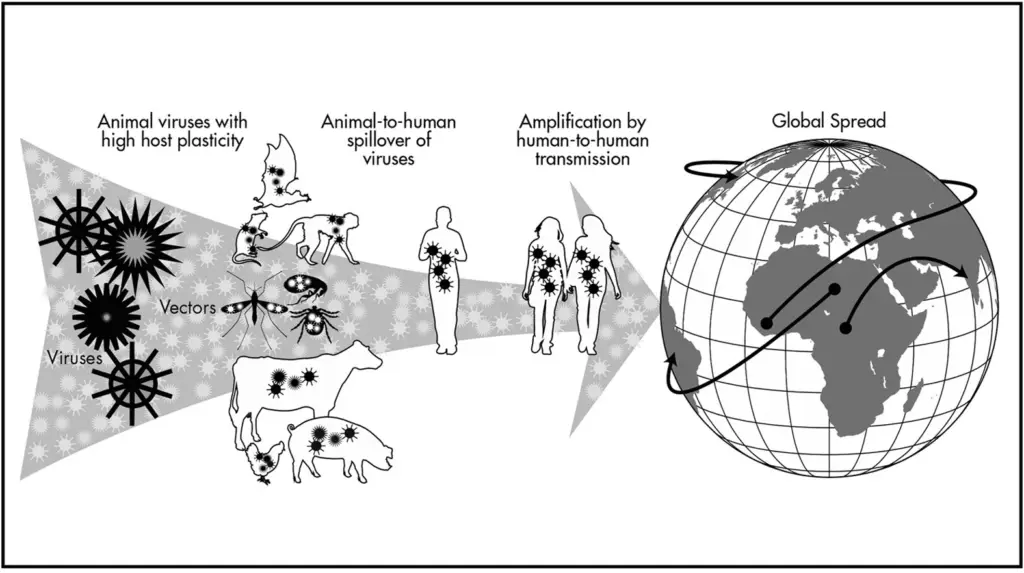
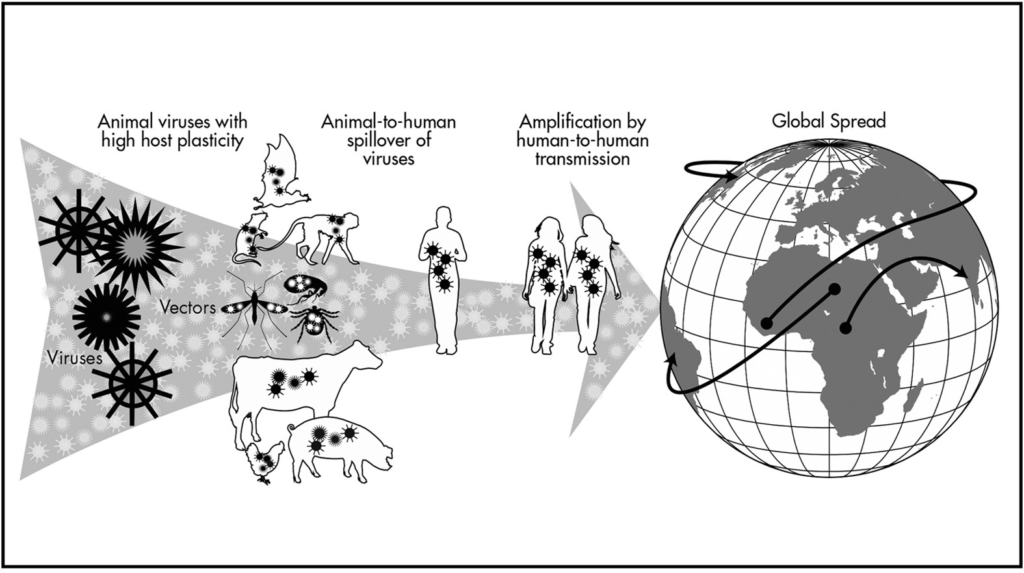
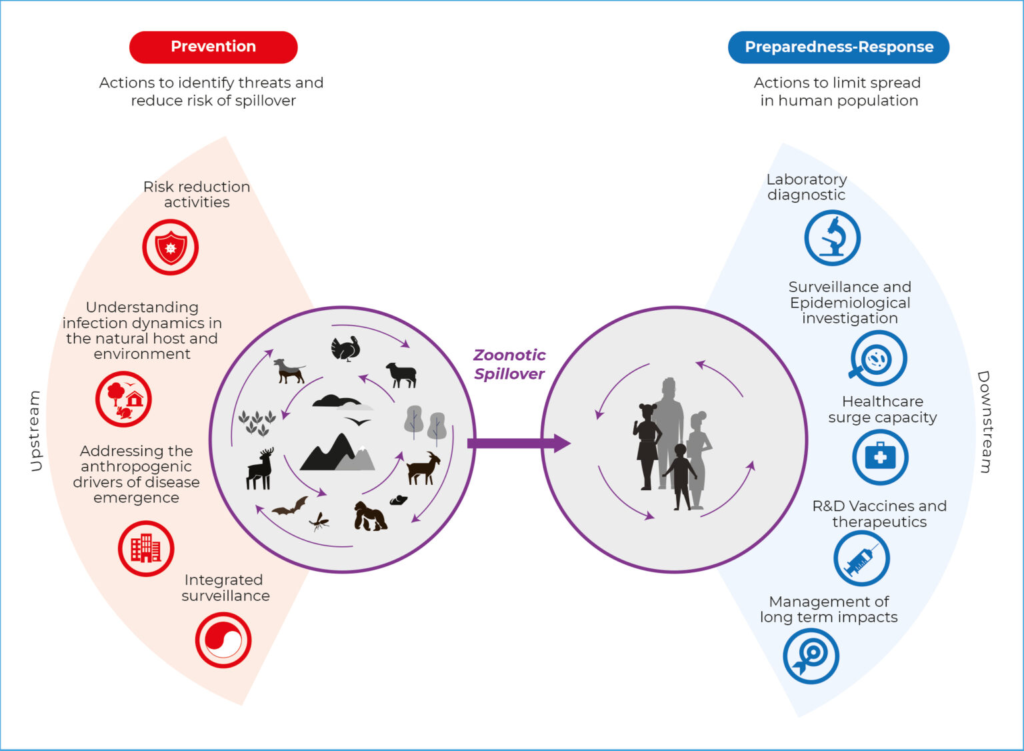
Before we explore the complexities of zoonotic disease spillover, let’s visualize how these events unfold. The diagram below, adapted from the Nature Journal article “Spillover and pandemic properties of zoonotic viruses with high host plasticity,” illustrates the key stages of Zoonotic Disease Spillover—from animal reservoirs to global transmission.
What is Zoonotic Spillover?
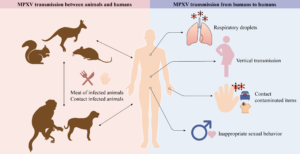
Zoonotic diseases, or zoonoses, are illnesses caused by microbes carried by animals that can spread to humans. Animals can transmit these diseases through various routes, including direct contact with blood or body fluids, vectors such as ticks and mosquitoes, and indirect contact with contaminated environments.
Spillover refers to an event where a pathogen is transmitted from a reservoir species (the animal host in which the pathogen naturally circulates) to another species. When this transmission occurs from an animal to a human, it is termed zoonotic disease spillover.
The pathogens that cause most emerging infectious diseases in humans originate in animals, particularly wildlife, and then spill over into human populations. This includes diseases like pandemic influenza, Ebola, mpox, and HIV/AIDS. SARS-CoV-2, the virus responsible for COVID-19, also likely emerged in humans through a spillover event.
Why it Matters?
The increasing frequency and impact of zoonotic diseases pose a significant threat to human and animal health, as well as global security. Over the recent decades, this threat has been on the rise due to factors such as population growth, climate change, and ecological disruption.
The majority of infectious disease threats we currently face are zoonotic, originating in animals and capable of transmission to humans through interactions between these groups. The consequences of Zoonotic Disease Spillover can be immense, as evidenced by the recent outbreaks of SARS-CoV-2, Ebola virus, Zika virus, MERS-CoV, and other emerging infectious diseases. These events have not only caused widespread illness and mortality but have also resulted in substantial economic losses, estimated in the trillions of dollars.
Furthermore, the potential for Zoonotic Disease Spillover to trigger global pandemics necessitates a proactive approach focused on prevention rather than solely relying on reactive measures. Strategies to reduce the probability of spillover events are often underprioritized despite evidence suggesting they are more cost-effective than solely focusing on response activities
Key Factors Driving Spillover Events
Zoonotic Disease Spillover is a complex process influenced by a confluence of ecological, epidemiological, and human behavioral factors. Understanding these drivers is essential for identifying high-risk scenarios and developing effective prevention strategies.
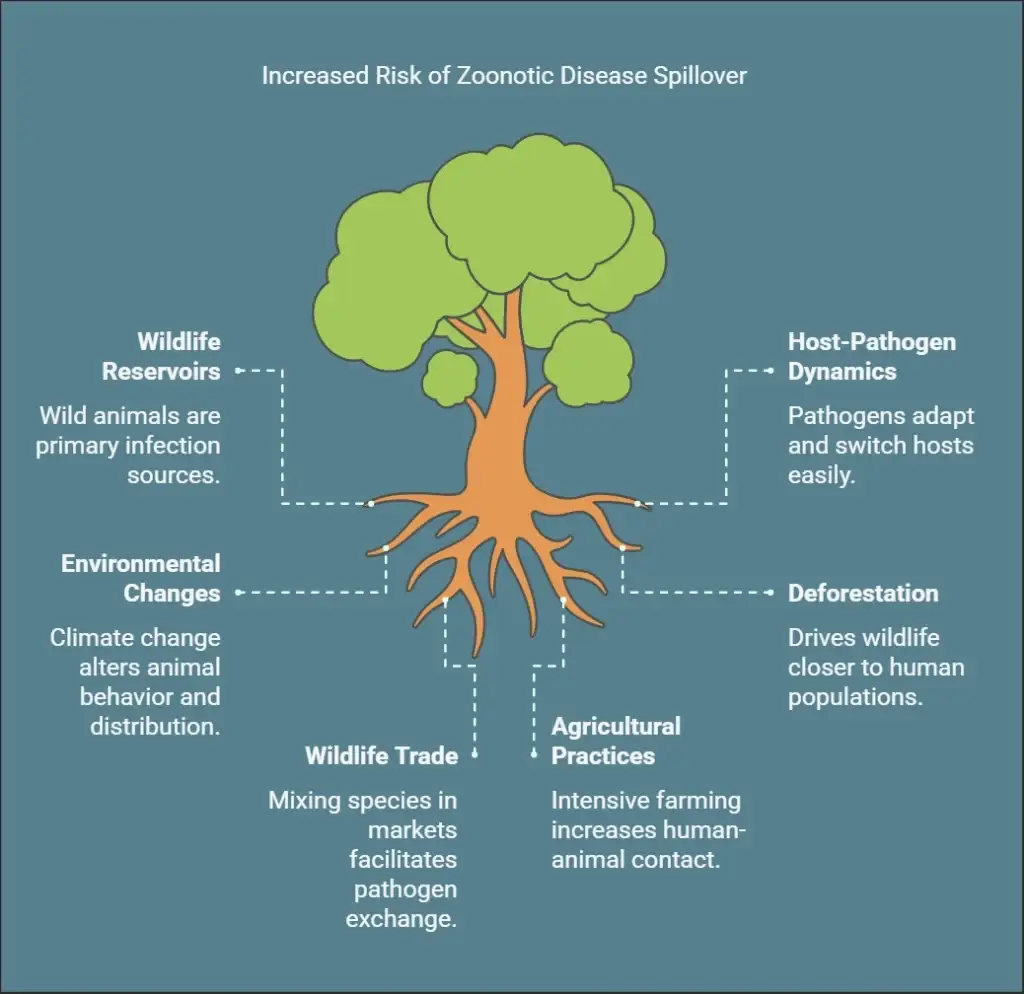
Wildlife Reservoirs: Identifying Potential Sources
Wild animals are increasingly recognized as the primary source of most emerging infectious disease events in humans. The vast diversity of wildlife on our planet harbors a rich pool of viruses, a fraction of which have the potential to adapt and infect humans.
Studies have shown that wild animals are significantly more likely to be the source of animal-to-human viral spillover compared to domesticated species. Certain animal groups have been implicated as reservoirs for a higher number of zoonotic viruses.
For instance, wild rodents have been identified as a source for a significant proportion of zoonotic viruses, particularly arenaviruses and bunyaviruses. Primates are frequently cited as the source of zoonotic retroviruses, while bats are more often implicated in the spillover of zoonotic paramyxoviruses and rhabdoviruses.
The concept of host plasticity, referring to the ability of a virus to infect a taxonomically and ecologically diverse range of hosts, is a crucial factor in determining the pandemic potential of zoonotic viruses. Viruses with high host plasticity are more likely to amplify Zoonotic Disease Spillover through secondary human-to-human transmission and achieve broader geographic spread.
Notably, viruses transmitted to humans during practices that facilitate the mixing of diverse animal species exhibit significantly higher host plasticity. Zoonotic viruses found in a greater number of animal host orders are significantly more likely to be transmissible between humans. This suggests that evolutionary selection for viruses capable of rapidly adapting to new hosts may also favor viruses capable of effective transmission within the new human host.
Host-Pathogen Dynamics: How Diseases Jump Species
The transmission of a pathogen or Zoonotic Disease Spillover from an animal to a human is not a straightforward process. It requires the pathogen to overcome a series of hierarchical barriers. These barriers encompass the ecological, epidemiological, and behavioral determinants of pathogen exposure, as well as the within-human factors that influence susceptibility to infection. If any of these barriers prove impenetrable, spillover cannot occur.
For some pathogens, successful spillover necessitates a narrow window of alignment across these barriers in space and time. In contrast, other pathogens with protracted environmental survival or wide dissemination may experience a more staggered alignment of these barriers.
Pathogens can achieve host switching through mechanisms such as rapid mutations, particularly observed in viruses like influenza A and avian flu. This adaptability broadens the range of potential host species for pathogen dispersal. Factors such as reservoir host density, pathogen prevalence within the reservoir population, and the intensity of infection in individual hosts all contribute to the pressure a pathogen exerts for Zoonotic Disease Spillover.
Human behaviors that influence exposure to potential pathogens, along with the integrity of within-human defenses against infection, are also critical determinants of Zoonotic Disease Spillover risk.
Environmental Changes and Spillover Risk
Human activities that drive climate change and cause ecological disruption are increasingly recognized as significant contributors to the risk of Zoonotic Disease Spillover. These changes can alter the distribution and behavior of both animal reservoirs and vectors, increasing the likelihood of contact with human populations.
Land-use change, including deforestation, agricultural expansion, and habitat fragmentation, is a major driver of emerging infectious diseases. The clearing and degradation of tropical and subtropical forests, in particular, create more frequent encounters between humans and domestic animals with wildlife, thereby increasing opportunities for pathogen spillover. These high-risk interfaces, often characterized by dense human and domestic animal populations living in close proximity to wildlife, account for a disproportionately high percentage of global Zoonotic Disease Spillover.
Interestingly, the relationship between biodiversity and disease transmission is complex. While some research suggests that increased host biodiversity might dilute pathogen transmission by reducing the probability of transmission among conspecifics, other studies indicate that human-dominated ecosystems with reduced biodiversity can actually lead to an increase in zoonotic host diversity and potentially higher spillover risk.
Habitat disturbance can also result in chronic stress and impaired health status in wildlife, potentially increasing their risk of becoming infected with or shedding viruses
Human Activities: Deforestation, Wildlife Trade, etc.
Several specific human activities significantly elevate the risk of Zoonotic Disease Spillover:
- Tropical Deforestation: The destruction of forests drives wildlife closer to human settlements and agricultural areas, increasing contact rates and spillover opportunities. Commercial exploitation of wildlife often intensifies following deforestation, further exacerbating the risk for Zoonotic Disease Spillover
- Illicit Wildlife Trade: Legal and illegal wildlife markets and trade pose a high risk for the emergence, amplification, and transmission of zoonotic pathogens. The close confinement and mixing of diverse wild animal species in these markets create ideal conditions for pathogen exchange and spillover. The demand for wild animals as food, pets, and for traditional medicines fuels this trade.
- Animal Husbandry: Intensive and high-density livestock farming, particularly when coupled with inadequate biosecurity measures, can facilitate the transmission of pathogens between domestic animals and wildlife, as well as to humans. The interface surrounding animal husbandry, such as large-scale swine and poultry production, represents an important area for spillover due to close interactions between workers and animals. Underfunded animal health services and household food insecurity can also drive risky husbandry practices that increase spillover risk.
- Agricultural Expansion and Intensification: Changes in land use for food production can profoundly alter human-wildlife interactions, sometimes suppressing contact with large predators but increasing contact with peridomestic species like rodents, which are common reservoirs for zoonotic pathogens
Case Study: Lessons from SARS-CoV-2
The COVID-19 pandemic serves as a stark reminder of the devastating potential of Zoonotic Disease Spillover and the critical need for robust prevention strategies.
Origin and Spread: Understanding SARS-CoV-2 Spillover
SARS-CoV-2, the virus that causes COVID-19, is widely believed to have originated in animals and subsequently spilled over into the human population. While the exact animal source is still under investigation, evidence points towards bats as a likely reservoir, with the possibility of an intermediate animal host involved in the transmission to humans. The emergence of the virus was likely facilitated by close contact between humans and animals, potentially in a wildlife market setting where various live and freshly slaughtered animals were sold. The rapid global spread of SARS-CoV-2 following the initial spillover event underscores the interconnectedness of the modern world and the speed at which a novel zoonotic pathogen can escalate into a pandemic.
Impact on Global Health: A Wake-Up Call
The COVID-19 pandemic has had a profound and multifaceted impact on global health. It has resulted in millions of deaths, overwhelmed healthcare systems worldwide, and caused significant long-term health consequences for many survivors. Beyond the direct health impacts, the pandemic has triggered widespread social and economic disruption, leading to job losses, business closures, and increased poverty.
The pandemic has also highlighted existing health inequalities and the vulnerability of global supply chains. The sheer scale of the COVID-19 crisis has served as a critical wake-up call, emphasizing the urgent need to prioritize pandemic prevention efforts and invest in strategies that address the underlying drivers of Zoonotic Disease Spillover.
Prevention and Mitigation Strategies
Preventing Zoonotic Disease Spillover at the animal-human interface is a core biosecurity goal. While preparedness for outbreaks is also essential, a greater emphasis on proactive prevention strategies is crucial for mitigating future pandemic threats
Next-Generation Surveillance and Early Warning Systems
Effective prevention requires robust surveillance systems that can detect potential spillover events early. This includes actively and passively monitoring areas where human, animal, and environmental interfaces create high-risk conditions. Pathogen surveillance efforts should encompass both human and animal populations, including wildlife and domestic animals, to understand the circulating zoonotic disease landscape.
Integrated surveillance systems that involve coordinated multisectoral efforts are particularly effective in providing insights into zoonotic pathogens in their natural reservoirs and tracking spillover events. Utilizing big data and associated analytical tools can enhance public health surveillance systems and facilitate the development of predictive models. Advances in machine learning and crowdsourcing can also offer opportunities to gather information about disease dynamics
Predictive Modeling and AI-Driven Risk Assessment
Predictive modeling plays an increasingly important role in anticipating and preventing zoonotic disease emergence. Big data-informed mapping techniques have the potential to predict disease outbreaks. By analyzing various ecological, environmental, and human behavioral factors, these models can help identify high-risk areas and potential Zoonotic Disease Spillover pathways. Artificial intelligence (AI) can further enhance risk assessment by processing vast amounts of data to identify patterns and predict future disease threats
Sustainable Land Use and Ecosystem Restoration
Addressing the environmental drivers of spillover is crucial for long-term prevention. Stopping the clearing and degradation of tropical and subtropical forests is a vital intervention. Sustainable land-use practices that minimize human encroachment into wildlife habitats and reduce habitat fragmentation can significantly lower spillover risk.
Ecosystem conservation and restoration efforts, such as reforestation, can play a crucial role in reducing the abundance of disease reservoirs in certain environments and mitigating spillover risk. Recognizing conservation as a security issue and investing in ecological preservation and restoration are essential steps.
Strengthening Global Health Security and Governance
Effective pandemic prevention requires strong global health security and governance frameworks. This includes fostering better integration between biological and ecological security approaches, breaking down funding silos, and promoting interdisciplinary collaboration.
International agreements, conventions, and treaties are essential for coordinating global efforts. Initiatives like PREZODE (Preventing Zoonotic Disease Emergence) exemplify collaborative, One Health-focused approaches to spillover prevention. Building sustained dialogue among policymakers, scientists, and practitioners across all levels is crucial for effective information sharing and rapid implementation of preventive measures
Behavioral Science and Public Engagement
Understanding and modifying human behaviors that contribute to spillover risk is a critical aspect of prevention. Community-designed interventions that are tailored to local contexts and address the health and economic security needs of communities living in emerging infectious disease hotspots are likely to be more effective in reducing human-wildlife contact.
Incorporating sociological expertise and integrating community preferences are essential for successful interventions. Public engagement and risk communication are also vital for building trust and ensuring the adoption of preventive behaviors
Public Health Interventions: Reducing Human-Wildlife Contact
Targeted public health interventions aimed at reducing direct and indirect contact between humans and wildlife are essential for preventing spillover. This includes shutting down or strictly regulating wildlife markets and trade, particularly those involving live and freshly butchered wild birds and mammals.
However, these measures must prioritize the rights and livelihoods of Indigenous Peoples and Local Communities (IPLCs) who may depend on wildlife for food and sustenance. Improving biosecurity in animal husbandry through investments in public and private animal health services and promoting the identification of animal illnesses of public health concern can decrease pathogen transmission between wildlife and domestic animals
Investment in One Health Infrastructure and Workforce Development
The One Health approach, which recognizes the interconnectedness of human, animal, and environmental health, provides a crucial framework for addressing zoonotic spillover. Investing in One Health infrastructure and workforce development is essential for building the capacity to effectively prevent, detect, and respond to zoonotic threats.
This includes fostering interdisciplinary collaborations, supporting research that integrates human, animal, and ecosystem health, and providing adequate funding for One Health initiatives. Lengthening the duration of funding for projects focused on ecosystem health and spillover prevention is necessary to collect longitudinal data and assess the long-term effectiveness of interventions
Future Research, Policy, and Innovation for Pandemic Preparedness
Continued progress in pandemic preparedness requires sustained research efforts, informed policymaking, and innovative solutions.
Identifying High-Risk Areas
Future research needs to focus on better identifying high-risk spillover areas by understanding the complex web of biological and ecological factors that contribute to spillover risks. This includes mapping potential pathogen circulation in wildlife and domestic animals. Standardizing data-related methods and practices across disciplines is crucial for enhancing the utility of research and informing policy recommendations
Global Cooperation and Policy Frameworks
Strengthening global cooperation is paramount for effective pandemic prevention. This includes developing and strengthening policies to discourage or reverse deforestation, combat the illicit wildlife trade, and promote sustainable practices in the livestock sector.
Policy frameworks should integrate a systems-thinking approach, considering the nexus between economic, demographic, and cultural factors that drive activities contributing to spillover risk. Incentivizing the reporting of livestock illnesses and deaths, particularly in low- and middle-income countries, is crucial for improving disease surveillance. Academic journals should be encouraged to publish negative or no-effect results to provide a more complete understanding of intervention efficacy
Takeaway Message: Protecting Human and Animal Health
Zoonotic disease spillover poses a significant and growing threat to global health security. The COVID-19 pandemic has underscored the catastrophic consequences that can arise from the emergence of novel zoonotic pathogens. However, this threat is not insurmountable.
By prioritizing primary prevention strategies that address the underlying drivers of spillover at the animal-human-environment interface, we can significantly reduce the risk of future pandemics. This requires a concerted effort grounded in the One Health approach, integrating ecological and biological security considerations, fostering interdisciplinary collaboration, and investing in sustainable solutions.
Protecting the health of animals and ecosystems is intrinsically linked to protecting human health. A proactive and holistic approach to preventing zoonotic spillover is not only a public health imperative but also a crucial investment in global well-being and security