Introduction
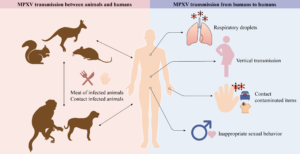
Deep in a Malaysian forest, a colony of fruit bats has lived undisturbed for half a century. A virus—Disease X—exists at low levels within a colony of fruit bats. For decades, it has remained largely unseen, a silent threat within its wildlife reservoir. This virus, through a chain of events driven by human actions—deforestation, shrinking habitats, food shortages for wildlife, and the proximity of newly established pig farms—finds its way to humans via pigs. The first human case occurs in a farmworker who recently attended a large family wedding, setting the stage for widespread transmission.
This all-too-familiar scenario is a stark reminder of how emerging infectious diseases often arise. It highlights the crucial interdependence of human, animal, wildlife, and environmental well-being—the very essence of the One Health approach, our best defense against future pandemics.
The One Health High Level Expert Panel (OHHLEP) defines One Health as
“an integrated, unifying approach that aims to sustainably balance and optimize the health of people, animals and ecosystems. It recognizes the health of humans, domestic and wild animals, plants, and the wider environment (including ecosystems) are closely linked and inter-dependent.”
This definition underscores the fundamental truth that human health, animal health, and environmental health are not separate entities but rather interconnected and mutually dependent. One Health promotes collaboration, coordination, and cooperation across diverse sectors—from medicine and veterinary science to ecology and environmental management—to tackle complex health challenges, especially those involving zoonotic diseases, fostering a more integrated and sustainable approach to well-being.
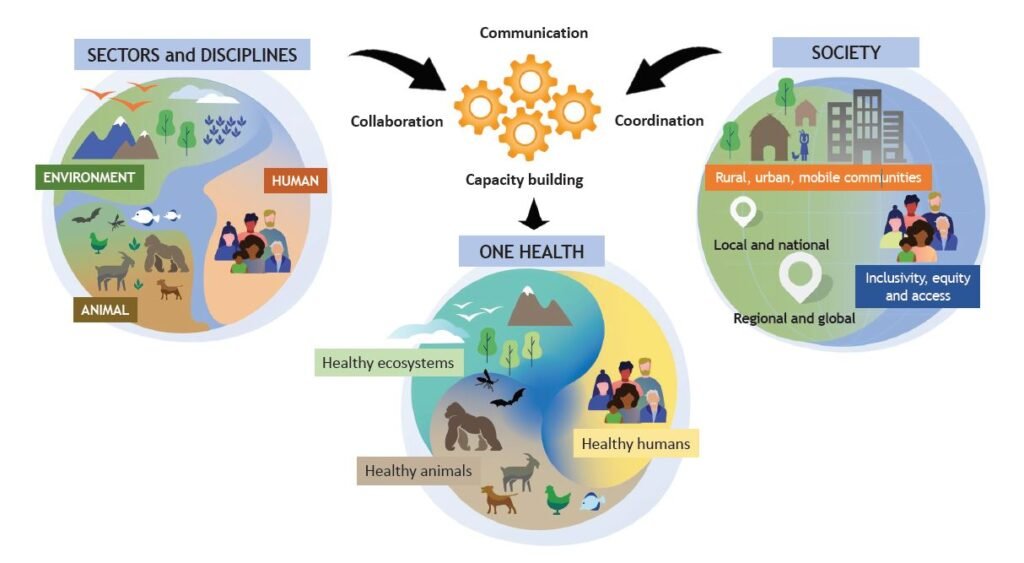
Figure: The One Health triad: Illustrating the interconnectedness of human, animal, and environmental health published in PLOS Pathogen
The Foundations of One Health
The scenario we explored earlier is a stark reminder of the interconnectedness of health and the power of the One Health approach. But it’s important to remember that this is just one example. One Health is not solely focused on emerging diseases. It’s a comprehensive strategy for addressing all health challenges that arise at the intersection of human, animal, and environmental well-being. From endemic diseases to neglected tropical diseases, viral to parasitic pathogens, One Health offers a framework for safeguarding health at every level. But how did this holistic approach come to be? Is it a modern invention? Let’s journey back in time to discover the history of One Health and examine its core principles.
Early History of One Health
The concept underpinning One Health—the interconnectedness of human, animal, and environmental health—is not a recent invention. While the term “One Health” may be relatively new, the recognition of these interconnections stretches back centuries, woven into the fabric of human understanding of health and well-being
- Early Veterinary Public Health: Even before recorded history, humans likely recognized the link between their health and the health of the animals they depended on for food, labor, and companionship. Observations of shared illnesses and the impact of environmental factors on both humans and animals likely formed the basis of early health practices. One of the earliest examples of this interconnected thinking can be seen in the work of Dr. Giovanni Maria Lancisi in the early 18th century. Appointed by Pope Clement XI to combat a devastating rinderpest outbreak in cattle, Lancisi recognized the link between animal disease and human well-being. His recommendation to cull infected and at-risk animals, a bold move for the time, demonstrated an understanding of disease control principles that are still relevant today. This marked an early milestone in recognizing the importance of controlling animal diseases to protect human populations.
- The Rise of Comparative Medicine: The 19th century saw the rise of comparative medicine, fueled by advances in pathology and a deeper understanding of disease mechanisms. Scientists began to recognize striking similarities between diseases affecting humans and animals. This era produced giants like Rudolf Virchow, a German physician and pathologist, who famously declared, “Between animal and human medicine there are no dividing lines—nor should there be.” Virchow’s work emphasized the value of studying diseases in animals to gain insights into human health and vice versa. He also coined the term “zoonoses” while studying the roundworm Trichinella spiralis in swine, further highlighting the connection between human and veterinary medicine. This concept of shared disease vulnerabilities across species was fundamental to the development of One Health thinking. William Osler, often called the “father of veterinary pathology,” was a Canadian physician with a deep interest in integrating human and animal health. Trained alongside both veterinarians and physicians, Osler recognized the interconnectedness of their fields. His early work, including his publication titled “The Relation of Animals to Man,” demonstrated his commitment to bridging the gap between human and animal medicine. This emphasis on interdisciplinary training and collaboration was a crucial precursor to the modern One Health approach.
- The Early Modern Age: Development of One Health: The late 19th and early 20th centuries witnessed the development of veterinary public health as a specialized field. Veterinarians played an increasingly important role in ensuring food safety, controlling zoonotic diseases, and protecting public health. This era saw the establishment of meat inspection programs and the recognition of the importance of veterinary expertise in safeguarding human populations from animal-borne diseases. Dr. Calvin W. Schwabe, considered the “father of modern veterinary epidemiology,” further advanced the One Health concept by coining the term “One Medicine” in his influential textbook, Veterinary Medicine and Human Health. Schwabe’s work emphasized the shared biological basis of disease in humans and animals, advocating for a unified approach to medicine.
These early developments laid the foundation for the modern One Health approach. They highlight the long-standing recognition that human, animal, and environmental health are interconnected and that a collaborative, interdisciplinary approach is essential for addressing complex health challenges. The stage was now set for formalizing the One Health concept and its expansion to include the crucial role of environmental health. This brings us to the modern era of One Health….
The Modern Era of One Health
The 20th and 21st centuries have witnessed a confluence of factors that have propelled the One Health approach to the forefront of global health discourse. The increasing recognition of the complex interplay between human, animal, and environmental health has solidified One Health as a crucial framework for addressing the health challenges of our time.
- The Rise of Zoonotic Diseases: The increasing recognition of the threat posed by zoonotic diseases – diseases that can be transmitted between animals and humans – has been a major catalyst for the One Health movement. Outbreaks of diseases like avian influenza (H5N1), SARS, MERS, and Ebola have underscored the interconnectedness of human and animal health and the need for a collaborative approach to disease surveillance and control.
- Environmental Change and Health: The growing awareness of the impact of environmental change on human and animal health has further strengthened the One Health perspective. Deforestation, climate change, and other environmental factors can disrupt ecosystems, increase contact between humans and animals, and create conditions that favor the emergence and spread of infectious diseases.
- Globalization and Trade: The increasing interconnectedness of the world through trade and travel has also played a role in the rise of One Health. The rapid movement of people, animals, and goods across borders can facilitate the spread of diseases, making international collaboration and a One Health approach essential for global health security
While the concept of interconnected health has long been recognized, the formalization of the “One Health” concept as a distinct approach gained significant momentum in the 21st century. Several key milestones mark this evolution:
- The Manhattan Principles (2004): In 2004, the Wildlife Conservation Society, in collaboration with Rockefeller University and other partners, convened a symposium that resulted in the Manhattan Principles. These 12 principles, focusing on the interface of human, animal, and ecosystem health, provided a foundational framework for the One Health approach, emphasizing the need for interdisciplinary collaboration to address emerging infectious diseases.
- Growing Recognition and Endorsement (2007-2008): The years 2007 and 2008 saw significant endorsements of the One Health concept. The American Medical Association and the American Veterinary Medical Association passed a joint resolution recognizing the interconnectedness of human, animal, and environmental health and the necessity of collaborative efforts. An international meeting in India, involving representatives from 111 countries and 29 international organizations, further promoted the adoption of One Health principles by governments.
- International Collaboration and Frameworks: A crucial outcome of these growing collaborations was the development of a strategic framework at the human-animal-environment interface by the United Nations System, including the WHO, FAO, UNICEF, OIE (now WOAH), and the World Bank. This framework provided a vital roadmap for coordinated action. In 2008, the concept gained further political traction with the development of “A Strategic Framework for Reducing Risks of Infectious Diseases at the Animal–Human–Ecosystems Interface” at the International Ministerial Conference on Avian and Pandemic Influenza in Egypt.
- The period from 2010 to 2013 marked a critical phase in the formalization and global adoption of the One Health approach. In 2010, the Tripartite (WOAH, FAO, WHO) published a concept note outlining a long-term strategy for international collaboration on health risks at the human-animal-ecosystem interface, while the Hanoi Declaration called for broad implementation of One Health. The Stone Mountain meeting in the same year identified key actions for translating the One Health concept into practice. In 2011, the first International One Health Congress convened, emphasizing the interdependence of human, animal, and environmental health. The following year saw the first One Health Summit in Davos, focusing on food safety and security. Finally, in 2013, the Second International One Health Congress, the largest to date, underscored the growing global commitment to this integrated approach.
- One Health has continued to evolve and gain global traction since 2013, solidifying its place as a crucial approach to health challenges. A major milestone was the establishment of the One Health High-Level Expert Panel (OHHLEP) in 2016, providing expert advice to international organizations. OHHLEP’s widely accepted definition of One Health emphasizes the interconnectedness of human, animal, and ecosystem health. 2 The annual One Health Day, first celebrated in 2021, has become a key event for raising awareness. The COVID-19 pandemic served as a stark reminder of the importance of One Health, demonstrating how a zoonotic virus can have devastating impacts across sectors. These recent developments highlight the growing recognition of One Health as an essential framework for addressing complex health challenges in an interconnected world.
Underlying Principles of One Health:
The successful implementation of One Health relies on a foundation of core principles that guide collaborative, multidisciplinary efforts. Central to this is the emphasis on communication, collaboration, coordination, and capacity building (the 4Cs), which are fundamental for translating theory into action within diverse settings. Building upon this, the One Health High-Level Expert Panel (OHHLEP), in an article published in One Health Outlook, has articulated six key underlying principles that further define the One Health approach:
- Equity between the sectors and disciplines; This principle underscores the importance of ensuring that all sectors and disciplines involved in One Health initiatives are treated fairly and have equal opportunities to contribute. It calls for the breakdown of traditional silos and the establishment of equitable partnerships.
- Sociopolitical and Multicultural Parity, Inclusion, and Engagement: Recognizing that health is influenced by social, political, and cultural factors, this principle emphasizes the need to ensure that all voices are heard and valued. It calls for the inclusion of marginalized communities and the consideration of diverse cultural perspectives in One Health decision-making. It can be referred as “Whole of a Society Approach” for implementing one health on the graound.
- Socio-ecological Equilibrium: This principle highlights the importance of maintaining a harmonious balance between human, animal, and environmental interactions. It acknowledges the intrinsic value of biodiversity, the need for access to sufficient natural resources, and the interconnectedness of all living things within ecosystems. Ulimately this principles acknowdge the interdependency and complex intaction with organism living in the earth
- Stewardship and Responsibility: This principle emphasizes the ethical responsibility of humans to act as stewards of the environment and to adopt sustainable solutions that promote animal welfare and ecosystem integrity. It calls for behavioral changes that benefit current and future generations.
- Transdisciplinarity and Multisectoral Collaboration: This principle underscores the need for collaboration among all relevant disciplines, including modern and traditional forms of knowledge. It calls for the integration of diverse perspectives to address complex health challenges.
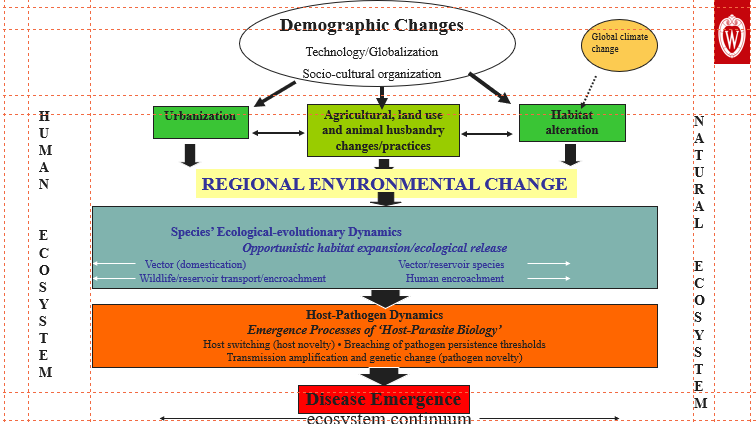
Drivers of Disease Emergence
We have discussed in detail the factors influencing the emergence of infectious diseases in the current world in the article on Why Emerging Infectious Diseases Are Rising: Key Drivers & Future Threats. In short, habitat alterations, deforestation, human population growth, biodiversity loss, and increasing factory farming often bring humans close to new pathogens, providing the chance of spillover or infecting susceptible hosts. These are complex processes of disease emergence which we can address through the One Health approach.
One Health in Practice: Case Studies and Applications
Having explored the definition, core principles, and underlying causes of disease emergence within the One Health framework, let’s now delve into its real-world applications and examine how it’s effectively managing health threats on the ground.
Case Study I: One Health Governance in Bangladesh
Bangladesh stands as an early adopter of the One Health approach, fostering multisectoral collaboration among government entities, including human health, animal health, wildlife, and agriculture sectors. A three-tiered coordination mechanism has been established, featuring a functional One Health secretariat within the government system. This unique, context-specific rotation of leadership among sectors, coupled with dedicated government funding, ensures the smooth operation of One Health initiatives through a "whole-of-government" approach. Activities encompass capacity building, outbreak investigation, joint surveillance, research dissemination, and data sharing among partners. A One Health strategic framework, initially developed in 2012 and subsequently updated, engages all stakeholders in Bangladesh. With the support of the CDC One Health Disease Prioritization Tool, the country has successfully prioritized One Health pathogens for focused action. This successful governance model has been featured in the Tripartite Guide to Addressing Zoonotic Diseases in Countries. We described this in publish article as Toward the Institutionalization of a One Health Agenda: What the World can Learn from Bangladesh
We’ve highlighted the importance of One Health in preventing emerging infectious diseases, especially in the developing world. Now, let’s explore a practical example: rabies control in Tanzania
Case Study II: Rabies Elimination Through Dog Vaccination in Tanzania
In Tanzania, a successful rabies control program exemplifies the One Health approach through its focus on mass dog vaccination. Studies have shown that achieving 70% vaccination coverage in domestic dogs effectively eliminates rabies, demonstrating both epidemiological and operational feasibility. Furthermore, this approach has proven cost-effective and has led to a decline in wildlife rabies cases where dog rabies was well-controlled. This demonstrates the interconnectedness of human, animal, and wildlife health, highlighting the power of a coordinated, community-engaged vaccination strategy (Cleaveland et al.,2018; Wallace et al.,2019)
These case studies illustrate the practical application and effectiveness of the One Health approach across diverse settings. However, scaling One Health implementation presents unique challenges and opportunities. In the following section, we will explore these complexities, focusing on multisectoral collaboration and diverse stakeholder engagement
Challenges in One Health Implementation
Implementing One Health initiatives effectively requires overcoming significant challenges. Firstly, inertia and resistance to change can hinder progress. As evident in the rabies control program in Tanzania (Cleaveland et al., 2022), maintaining consistent vaccination coverage requires overcoming resistance to change within communities and ensuring sustained effort.
Moreover, working in diverse environments has the potential for dissent and disagreement among team members from different sectors, leading to negative feelings and hindering collaboration. This is further emphasized by the historical context of One Health which shows how the separation of human and animal health disciplines has historically hindered progress.
Secondly, institutional barriers, such as siloed government agencies, inadequate funding, and insufficient data sharing, can impede intersectoral collaboration and hinder the effective implementation of One Health strategies.
Opportunities for One Health Success
Despite these challenges, the approach presents numerous opportunities. By fostering strong communication and building trust among diverse teams, we can overcome challenges related to diverse perspectives and ensure effective collaboration. Investing in capacity building, strengthening surveillance systems, and leveraging technology can significantly enhance One Health implementation. Furthermore, learning from successful case studies, such as the rabies control program in Tanzania, can provide valuable insights and inform future One Health initiatives. By addressing these challenges and leveraging these opportunities, we can harness the full potential of the One Health approach to safeguard global health and well-being.