I started my career as a Veterinary Epidemiologist working on outbreak investigations and preventing zoonotic pathogen spillover from wildlife to humans and animals. Later, I transitioned to the disease ecology department, working on understanding the spatiotemporal pattern of host behaviors and how it shapes the dynamics of environmentally transmitted pathogens like anthrax, chronic wasting disease, Nipah encephalitis, etc.
I realized that understanding the complex interactions between pathogens and their environments is crucial in the ever-evolving world of infectious diseases. Knowing how pathogens emerge and persist in ecosystems provides valuable insights into public Health, wildlife conservation, and ecosystem management.
I am sure you might also wonder why diseases like COVID-19, Ebola, or Lyme explode into human populations and what factors allow the pathogens to persist in ecosystems long after the headlines fade.
The answers lie in disease ecology, which studies how pathogens (e.g., viruses, bacteria, parasites, etc.) interact with their host environment and colonize within the host, sometimes with high virulence (severity of the infection) capacity and sometimes with less pathogenicity.
In this post, we’ll explore the mechanisms behind pathogen emergence, the secrets to their persistence, and why understanding these dynamics is critical for public health and conservation.
The Basics of Disease Ecology
As mentioned earlier, Disease ecology is a science at the intersection of biology, epidemiology, and environmental science. To me, it’s like studying the social life of microbes—who they hang out with, where they love to live, and how they make new friends (or enemies)!
At its core, disease ecology looks at the following:
- How pathogens transmit and spread over space and time
- The impact of pathogens on host populations
- The role of environmental factors in disease dynamics
By studying these interactions, “a disease ecologist” can predict outbreaks, mitigate risks, and even prevent future pandemics. Think of it as a detective story in which we try to understand the “who, what, where, when, and why” of disease outbreaks.
The Emergence of New Pathogens
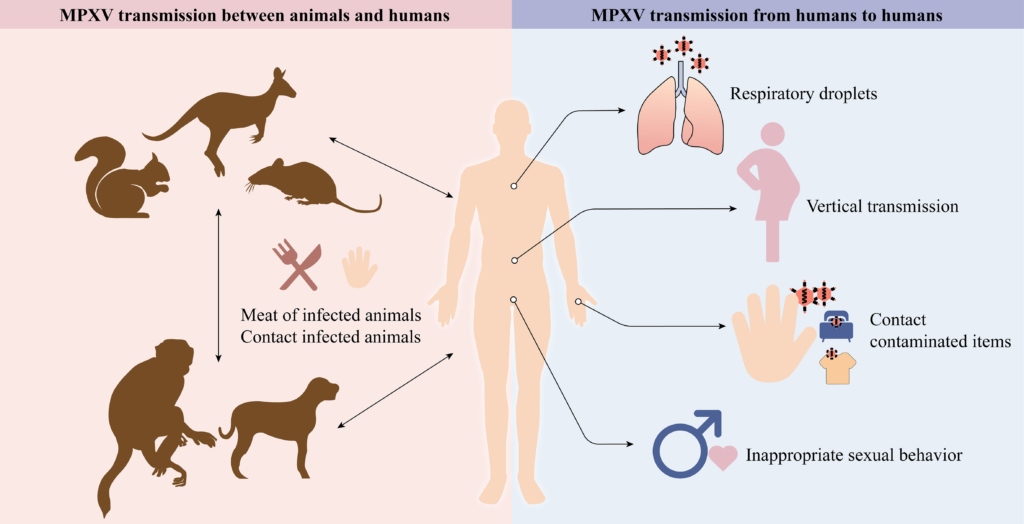
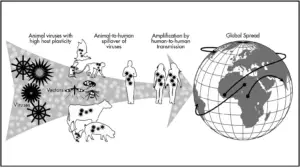
Let’s start with the basics—how pathogens emerge. It is estimated that more than 60% of emerging infectious diseases are of animal origin, while 75% of these pathogens originated in wildlife (Jones et al., 2008). But the process of pathogens infecting humans isn’t simple—it’s not as simple as a bug suddenly deciding to infect humans because it’s bored! Disease emergence is a complex process involving multiple steps and factors.
The Spillover Event
The first step of pathogen emergence is called “spillover,” when a pathogen jumps from one species to another by breaking the cross-species barrier. This phenomenon is more common in zoonotic diseases, where animal pathogens infect humans. Surprisingly, biodiversity plays a dual role in this disease-emergence process.
- As a source pool, more diverse ecosystems may harbor a greater variety of potential pathogens.
- As a buffer: Higher biodiversity can sometimes reduce disease transmission through the “dilution effect.”
Factors Influencing Emergence
Emerging infectious diseases are occurring at a higher rate than ever before. Several factors can increase the likelihood of pathogen emergence:
- Land use changes: Deforestation and agricultural expansion can bring humans closer to wildlife reservoirs.
- Wildlife trade: This can create opportunities for pathogens to jump between species.
- Climate change: Altering ecosystems can shift the range of both hosts and pathogens.
You May Also Like
Persistence of Pathogens in Ecosystems
Once a pathogen has emerged, how does it stick around? This is where the concept of ecological succession comes into play.
Ecological Succession in Disease
Just as plant communities undergo succession over time, pathogen communities within hosts may follow a similar pattern. This idea suggests that specific pathogens may be more likely to infect hosts at different stages of their lives.
For example, some pathogens might be “early colonizers,” infecting young hosts, while others might be “late-stage” pathogens, more common in older individuals.
The Role of Host Populations
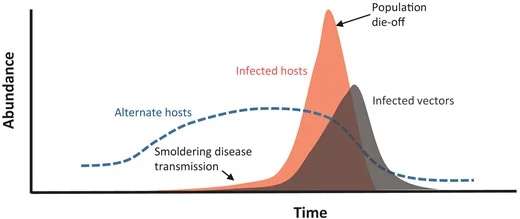
Pathogens are not isolated—they’re part of a complex ecosystem involving hosts, vectors, and the environment. A pathogen’s persistence often depends on the dynamics of its host population.
Consider the case of plague in prairie dog colonies:
Vectors: The Middlemen of Disease
Mosquitoes, ticks, and fleas transmit pathogens while feeding on multiple hosts. Diseases like malaria and Zika rely entirely on these vectors to survive, which is why mosquito control is so vital.
Environmental Survival
Some pathogens thrive outside hosts. Vibrio cholerae (cholera) persists in water, while anthrax spores survive in soil for decades. Not all pathogens operate the same way. Their survival depends on traits like transmission routes, host range, and environmental resilience. Let’s break this down with a table:
| Pathogen | Reservoir Host | Transmission Route | R0 | Environmental Stability |
|---|---|---|---|---|
| Influenza | Birds, Swine | Airborne | 1–2 | Low (dies on surfaces) |
| Ebola | Bats | Bodily fluids | 1.5–2.5 | Moderate (weeks in fluids) |
| Lyme Disease | Mice, Deer | Tick bite | 3–4 | High (survives in ticks) |
| Cholera | Aquatic environments | Contaminated water | 2–5 | High (months in water) |
Implications for Disease Management
Understanding disease ecology has significant implications for managing and controlling infectious diseases in susceptible populations.
The Offensive vs. Defensive Approach
One interesting concept borrowed from invasive species management is the idea of “offensive” versus “defensive” strategies.
- Offensive strategies: Focus on limiting the dispersal of a pathogen from established sites.
- Defensive strategies: Aim to reduce the vulnerability of uninfected areas to colonization.
This approach requires a deep understanding of whether a pathogen community is dispersal-limited, niche-based, or random in its assembly.
Community Ecology Tools
Recent advances in community ecology offer powerful tools for understanding and managing infectious diseases. These tools can help:
- Identify factors governing complex assemblages of hosts, parasites, and vectors
- Reveal how processes link across scales from individual hosts to regions
- Determine drivers of heterogeneities among individuals, species, and regions
Adopting these approaches can enhance disease management strategies and target control efforts more effectively (Johnson et al. 2016)
Implications for Public Health and Conservation
The One Health Approach
Disease ecology underscores the need for One Health—a collaborative framework linking human, animal, and environmental health. For example:
- Vaccinating dogs reduces rabies risk in humans (WHO, 2023).
- Protecting forests limits spillover by preserving natural barriers between wildlife and people.
Climate Change as a Disease Amplifier
Warmer temperatures are accelerating vector lifecycles and shifting their habitats. A 2023 study found that Aedes aegypti mosquitoes, which carry dengue, have expanded their range by 13% since the 1950s due to climate shifts (Carlson et al., 2023).
The Role of Biodiversity
Paradoxically, diverse ecosystems often suppress disease spread. For example, in the Amazon, high mammal biodiversity dilutes the effect of Lyme disease reservoirs, reducing human risk (Civitello et al., 2015). This “dilution effect” highlights why conservation is a public health strategy.
Take-home message:
Disease ecology offers a fascinating lens through which to view the complex world of infectious diseases. By understanding the ecological context in which pathogens emerge and persist, we can develop more effective disease prevention and control strategies.
As we continue to face global health challenges, from emerging zoonotic diseases to the impacts of climate change on disease dynamics, the insights from disease ecology will be more critical than ever. It reminds us that in the intricate web of life, even the smallest organisms can profoundly impact ecosystems and human health.
So the next time you hear about a disease outbreak, remember – it’s not just about the pathogen but the entire ecological stage on which it performs. In the grand theater of nature, disease ecology helps us understand the script, the actors, and the complex interactions that shape the drama of infectious diseases.
The Future of Disease Ecology
As we continue confronting emerging infectious threats, disease ecology will play an increasingly vital role in shaping our understanding and response strategies. The question now is: What should be our research priorities moving forward? How can we better integrate disease ecologists into mainstream health research and policymaking?
The answers lie in our collective effort to bridge disciplines — and, perhaps, your following conversation.