Five years ago, the world stopped. Just stopped!
Cities went quiet, doors shut, and a fear of uncertainty mounted in the sky. Every morning we wake up with news of “numbers”—which essentially means a person died or was infected with COVID-19. Social structure, business, economy, emergency services—everything was in halt.

COVID-19 dashboard, which was probably the most visited site during the pandemic
Today, after 5 years, the silence breaks with a wake-up call on different diseases: bird flu spreading like wildfire, strange illnesses popping up in far-off villages. The programs that were supposed to ensure our “collective” health and global health security are being cut back, and the scientists and professionals who are on the front line to protect the health of humans, animals, and the environment are being silenced. This is all happening when the chance of emerging infectious diseases is higher than ever before. All this together has kept me wondering: are we inviting another pandemic like COVID-19?
We experienced the devastating impact of a pandemic, but can we really imagine something worse? Something with the speed of COVID-19 and the deadliness of Ebola? This article will explore these recent events, the fears they raise, and why we’re failing to ensure global health security. We’ll look at how these actions are setting the stage for a pandemic the world is simply not prepared for.
COVID-19 and the Lessons We Failed to Learn
During the COVID-19 pandemic, I worked within a public health emergency response organization. I witnessed firsthand how COVID-19 revealed critical weaknesses in public health infrastructure, emergency response, global cooperation, vaccine equity, and pandemic preparedness. From supply chain disruptions, hindering the delivery of desperately needed medical equipment like oxygen and simple masks, to overwhelmed healthcare workers struggling to provide care with minimal PPE, the strain was immense.
While the pandemic’s acute phase has passed, and people adapt to a “new normal,” the economic repercussions persist. The impact of the COVID-19 pandemic is hard to describe in writing; for further details, refer to the joint statement of the ILO, FAO, IFAD, and WHO. Billions were invested in vaccine development and response measures, yet many nations have failed to sustain these systems. The swift dismantling of pandemic preparedness programs—particularly in the U.S., where USAID’s global health budget faces significant cuts—fuels anxiety that the world will once again be unprepared for the next crisis.
Current Global Health Threats: A Perfect Storm?
The reality is stark: emerging infectious diseases are becoming more frequent, a trend expected to accelerate. Let’s examine the convergence of critical threats that have surfaced in the past five years. Since the onset of the COVID-19 pandemic, several infectious disease events with pandemic potential have emerged, prompting Public Health Emergency of International Concern (PHEIC) alerts. Notable examples include::
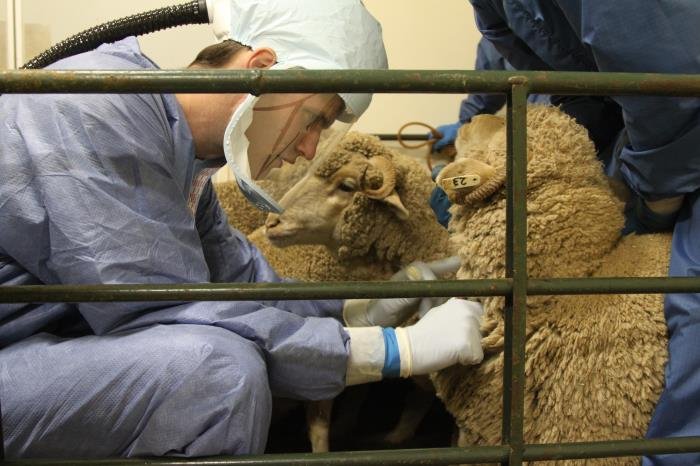
Mpox (Monkeypox):
In August 2024, the World Health Organization (WHO) declared mpox a public health emergency due to a more lethal variant primarily affecting children, especially in the Democratic Republic of Congo. Isolated cases were also reported in Sweden and Thailand, indicating potential for wider spread. Vaccination efforts faced challenges due to limited supplies and inequitable distribution.
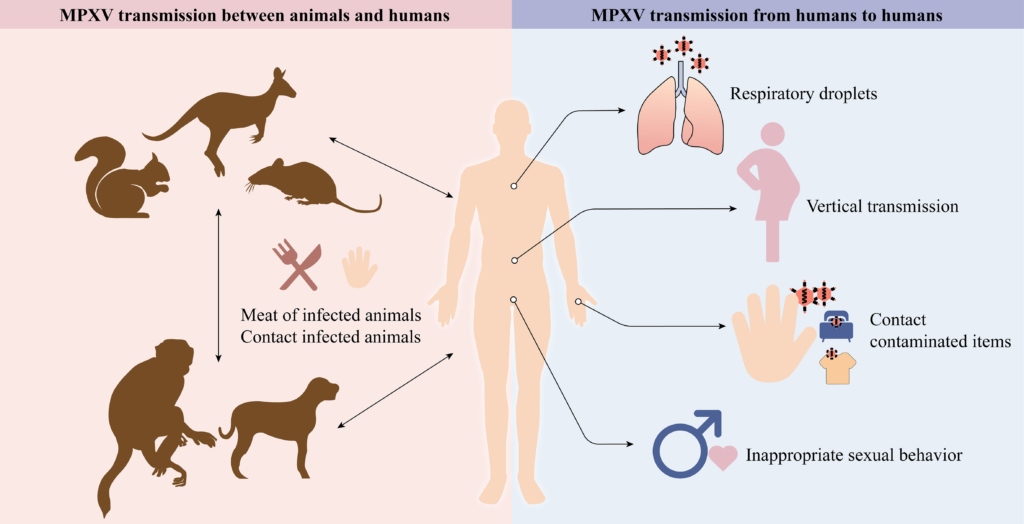
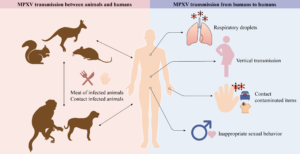
Possible Transmission Routes and Mechanisms of Monkeypox Virus (MPXV) Between Animals and Humans described by Wang et al.2023
According to WHO’s latest temporary recommendations issued in February 2025, emphasis has been placed on strengthening emergency coordination, enhancing sensitive and geographically comprehensive surveillance, expanding diagnostic capabilities, and scaling up targeted vaccination efforts, especially in hotspots experiencing sustained transmission. Additional recommendations include investing in genomic sequencing, addressing research gaps to understand zoonotic spillovers, and promoting community engagement to reduce stigma and misinformation, ensuring response measures respect human rights and dignity
H5N1 Bird Flu Outbreak
Avian Influenza (bird flu), ongoing since 2022, raised global pandemic potential alarms as the virus crossed species barriers and adapted to mammalian hosts, including dairy cattle, resulting in widespread exposure and sporadic human illness. Although most human cases have been mild, H5N1 has demonstrated the potential for severe disease.
Experts highlight significant challenges in rapidly developing and scaling up influenza vaccines, constrained by current protein-based technologies and regulatory bottlenecks. They recommend urgent global action, including the adoption of newer technologies such as mRNA vaccines, streamlined regulatory processes, and improved global collaboration among industry, governments, and regulators.
Pandemic preparedness initiatives should be urgently resourced and implemented, with comprehensive planning that incorporates societal engagement and addresses vaccine hesitancy, misinformation, and logistical challenges, thereby strengthening readiness and minimizing the risk of severe societal impacts
Marburg Virus:
Marburg virus caused a significant outbreak in Rwanda in early 2024, resulting in 66 confirmed cases, with 13 deaths (as of November 2024). Health care workers from two health centers accounted for nearly 80% of all cases. Most cases occurred in Kigali city, especially during the initial weeks (epidemiological weeks 39–41), followed by a sharp decline. No new confirmed cases were reported after 1 November 2024. Surveillance efforts continued, including regular PCR testing and monitoring of 470 contacts. Rwanda initiated a 42-day countdown period to officially declare the outbreak over, provided no new cases emerge during this time. The WHO continues supporting Rwanda through enhanced surveillance and infection prevention and control measures until the outbreak is officially declared concluded.
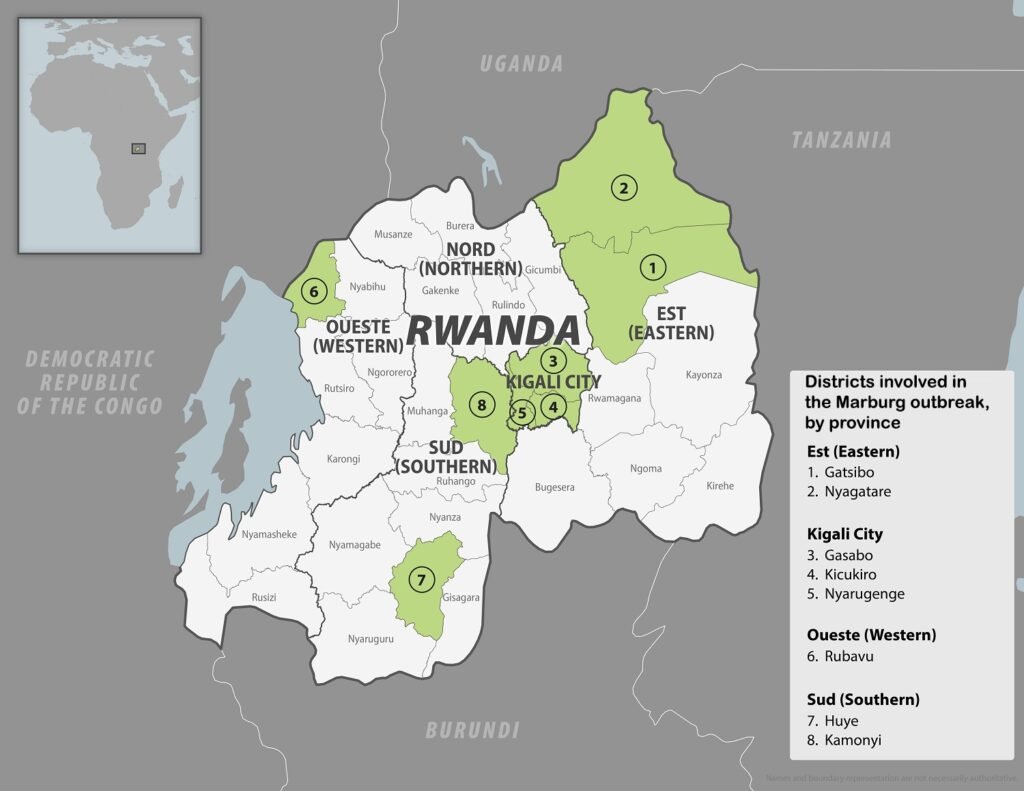
2024 Marburg outbreak in Rwanda from CDC
Human Metapneumovirus (HMPV):
Human Metapneumovirus (HMPV) has shown increased activity during late 2024 and early 2025, especially in the temperate Northern Hemisphere, including northern China. While elevated acute respiratory infections (ARI) and influenza-like illnesses (ILI) rates have been observed, this follows expected seasonal patterns rather than unusual outbreak patterns.
Although some HMPV cases may require hospitalization due to complications such as bronchitis or pneumonia, most infections are mild, presenting upper respiratory symptoms similar to a common cold, with recovery occurring within a few days. Co-circulation of multiple respiratory pathogens, including influenza and SARS-CoV-2, has placed added pressure on health care systems.
However, according to WHO, there have been no reports of unusual outbreak patterns, and Chinese authorities indicate that health care systems have not been overwhelmed, nor have emergency measures been triggered. Ongoing monitoring and surveillance by WHO continue at global, regional, and country levels (WHO Flu Chart)
Measles outbreak in USA:
United States experienced a resurgence in the United States in 2024–2025, with 285 cases reported across 33 jurisdictions in 2024, and 222 cases across 12 jurisdictions reported by March 2025. Most cases involved individuals who were unvaccinated or had unknown vaccination status (94% in 2025). There were significant hospitalization rates, particularly among children under five (28% in 2025). In 2025, three outbreaks accounted for 93% of cases. One confirmed death and another under investigation occurred in 2025. The outbreak underscored risks associated with declining vaccination rates post-COVID-19, highlighting the importance of maintaining high immunization coverage. Please refer to CDC measles website for the latest updates
Having all these viral disease outbreaks underscores a broader pattern of emerging infectious diseases, highlighting significant vulnerabilities in global health security. These outbreaks illustrate the urgent need for continuous surveillance, timely public health interventions, and equitable access to medical resources. Additionally, they emphasize the importance of understanding zoonotic disease transmission, a topic explored extensively in discussions about the emergence and management of zoonotic diseases.
Global Health at Risk: The Impact of Weakened Coordination
The freezing of USAID global health funds has severely impacted outbreak response efforts, particularly in Africa and Asia. This has delayed critical support for combating Ebola, Marburg virus, Nipah encephalitis and other emerging infectious diseases, leaving vulnerable populations at greater risk.
The U.S. withdrawal from the World Health Organization (WHO) has further weakened international pandemic coordination, disrupting global disease surveillance, vaccine research, and emergency response efforts. As threats from H5N1, Ebola, and antimicrobial resistance (AMR) continue to grow, the decision to scale back engagement with WHO has reduced the world’s ability to respond to future pandemics effectively.
Meanwhile, the H5N1 avian influenza outbreak has continued to spread, affecting poultry, dairy cattle, wild birds, and domestic pets. The virus’s increasing ability to jump between species raises concerns over a potential spillover event into humans. However, public health response efforts remain undermined by workforce reductions and funding cuts, limiting the ability to contain the spread.
At the same time, new Ebola cases in the Democratic Republic of Congo and Uganda have sparked fears of another regional outbreak. Adding to the concern, a mysterious hemorrhagic fever outbreak in West Africa has resulted in over 60 reported deaths. These outbreaks indicate that global disease surveillance is failing in critical areas, largely due to funding shortages and weakened health infrastructure.
Budget cuts targeting NIH, CDC, and pandemic research programs have further exacerbated these challenges, leaving major gaps in early detection and rapid containment of emerging infectious diseases. The reductions have directly affected the development of vaccines, diagnostic tools, and response strategies, increasing the risk of delayed interventions ultimately affecting the America First Agenda
Compounding these vulnerabilities, the CDC’s decision to lay off Epidemic Intelligence Service (EIS) officers—the frontline workforce responsible for detecting and responding to disease outbreaks—has significantly weakened public health readiness. With fewer trained epidemiologists monitoring global disease trends, the likelihood of undetected outbreaks escalating into large-scale health crises has risen.
As these compounding crises unfold, experts warn that the world is becoming increasingly vulnerable to the next pandemic. The combination of reduced funding, weakened surveillance, declining global cooperation, and workforce reductions has created an environment where emerging threats may go undetected until it is too late to contain them.
Global Health Security is National Security
A growing body of evidence underscores that global health security is inextricably linked to national security. The recent article from The Telegraph highlights how pandemic preparedness is not just a public health issue but a matter of geopolitical stability. The COVID-19 pandemic, the ongoing H5N1 outbreak, and emerging threats like Ebola have demonstrated that failing to invest in global health infrastructure directly threatens economic resilience, supply chains, and national security interests.
The article warns that neglecting vaccine production, disease surveillance, and international coordination makes nations more vulnerable—not only to pandemics but also to bioterrorism threats and economic destabilization. With USAID funding halted, WHO partnerships weakened, and domestic public health budgets slashed, countries are leaving themselves exposed to a future where pandemics are deadlier and more disruptive.
The Next Pandemic: A Crisis Waiting to Happen
The warning signs are clear, yet history seems doomed to repeat itself. Five years ago, COVID-19 caught the world off guard, exposing deep vulnerabilities in our global health system. We promised never to be unprepared again, yet today, as H5N1 spreads, Ebola resurges, and antimicrobial resistance rises, the very systems meant to protect us are being dismantled.
Budget cuts to pandemic response programs, the weakening of global coordination through WHO withdrawal, and the layoffs of epidemic intelligence officers are not just policy choices—they are deliberate steps toward vulnerability. Instead of fortifying pandemic defenses, we are systematically undoing the progress made after COVID-19, inviting disaster.
Public perception remains dangerously complacent. Few are alarmed by H5N1, just as few paid attention to COVID-19 before it exploded into a global crisis. The difference now is that we should know better. Yet, governments continue to defund preparedness, erase public health data, and silence scientific warnings. If COVID-19 was a wake-up call, the world seems to be hitting snooze.
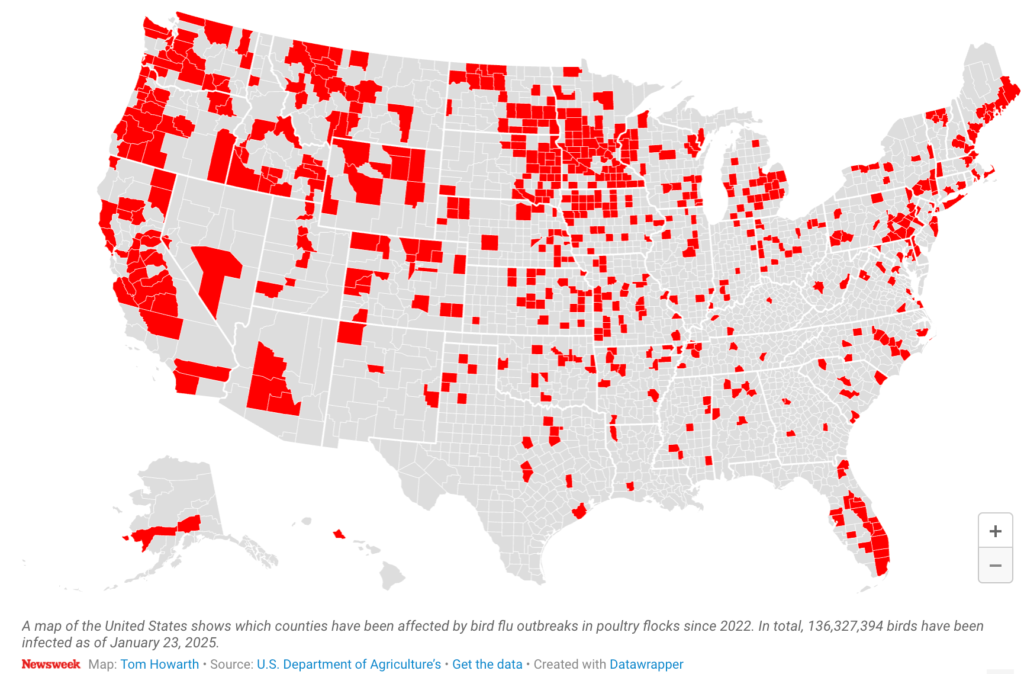
A map showing the rapid spread of H5N1 across the United States, coupled with a graph illustrating the drastic drop in global health funding, tells a story words alone cannot convey. The numbers are stark, the trajectory alarming. Each day we delay, each dollar we cut, brings us closer to a crisis we could have prevented.
The next pandemic is no longer a question of if—but when. And when it arrives, the record will show that we had every opportunity to prevent catastrophe, but chose instead to turn away, dismantle protections, and let history repeat itself.
The world had a chance to build resilient pandemic defenses after COVID-19, but instead, short-sighted policy decisions are making another global health crisis more likely. Ignoring emerging outbreaks, cutting science budgets, and erasing public health data will not prevent the next pandemic—it will only ensure we are unprepared when it arrives.
With H5N1 spreading across mammals, Ebola resurging, and new viral threats emerging, we should be expanding, not dismantling, our preparedness infrastructure. Instead of rolling back public health programs, policymakers must recognize that investment in science, surveillance, and global cooperation is the best insurance policy against future pandemics.
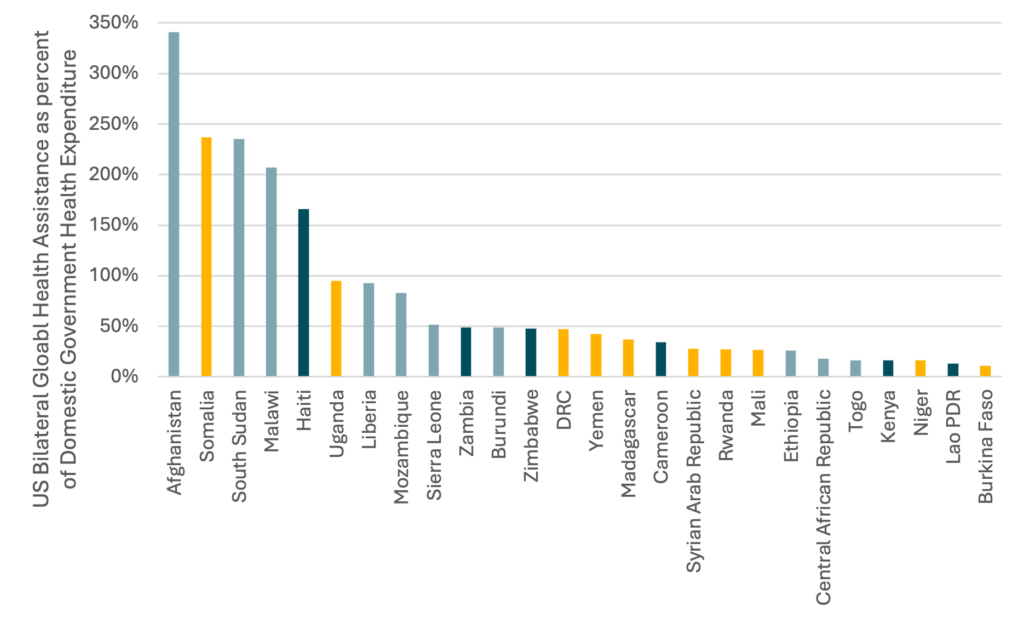
26 Vulnerable Countries at Risk as US Aid Cuts Create an Unfillable Gap
A Call to Action
On this five-year remembrance of COVID-19, the world stands at a crossroads. Will we take the necessary steps to prevent history from repeating itself, or will we ignore the warning signs and invite the next pandemic closer? The choices we make today will define global health security for decades to come.
Now is the time to restore funding for pandemic preparedness, strengthen surveillance systems, and prioritize transparency in public health data
—before it’s too late.